Scaling a private practice means expanding your capacity and capabilities in a sustainable, quality-driven way, not just seeing more patients, but building systems that support growth without burnout. Whether you're a solo practitioner or managing a group practice, strategic scaling creates financial resilience, operational efficiency, and the ability to serve more patients while maintaining exceptional care standards.
Let’s take a look at proven frameworks, automation strategies, and data-driven metrics that transform practices from reactive to proactive, ensuring long-term growth anchored in both clinical excellence and business intelligence.
Understanding the Importance of Scaling Your Private Practice
Scaling extends far beyond simply increasing patient volume. It represents a fundamental shift in how your practice operates, creating systems that multiply your impact without proportionally increasing your workload or compromising care quality.
When executed thoughtfully, scaling generates multiple revenue streams, builds operational redundancy that protects against market fluctuations, and establishes the infrastructure needed for sustainable growth.
The financial benefits are compelling. Scaled practices typically achieve higher profit margins through operational efficiencies, better negotiating power with suppliers and insurers, and diversified service offerings that capture more value per patient relationship.
Beyond revenue, scaling enables you to invest in better technology, attract top talent, and create career pathways that reduce staff turnover. From a patient care perspective, scaling done right means more access to your services, shorter wait times through optimized scheduling, and the resources to invest in cutting-edge treatments and diagnostic tools.
The key distinction between healthy scaling and unsustainable growth lies in building systems that preserve the personalized, patient-centered approach that likely defined your early success while leveraging technology and team development to extend your reach.
Embracing Automation to Streamline Practice Operations

Administrative tasks consume an outsized portion of healthcare practice resources, often pulling clinical staff away from patient-facing activities. Automation addresses this drain by handling repetitive, rules-based processes with speed and consistency that human staff cannot match.
Start with appointment management. Automated reminder systems via text, email, or voice calls reduce no-show rates by 20–30%, directly impacting revenue and schedule efficiency. These systems can also handle rescheduling requests, waitlist management, and confirmation workflows without staff intervention.
Appointment reminder and billing automation tools streamline practice operations and allow staff to address more complex patient needs.
Billing and insurance verification represent another high-impact automation opportunity. Modern systems can automatically verify coverage before appointments, flag eligibility issues, submit claims electronically, and follow up on denials - tasks that traditionally required dedicated billing staff hours. This reduces claim rejection rates and accelerates payment cycles.
Patient communications benefit enormously from automation. Post-visit surveys, educational content delivery, medication reminders, and care plan check-ins can all be triggered automatically based on appointment types or patient conditions. This consistency improves patient engagement while freeing your team to handle conversations that truly require human judgment and empathy.
The cumulative effect of these automations is profound. Practices typically reclaim 10-15 hours per week of staff time, reduce administrative errors by 40-50%, and improve patient satisfaction scores through more reliable, timely communications. This efficiency gain creates the bandwidth needed to serve more patients or invest in higher-value activities like care coordination and patient education.
Leveraging AI Solutions for Efficiency and Revenue Growth
Artificial intelligence in healthcare refers to computer-driven technology that simulates human cognitive tasks, from pattern recognition to decision support, enabling practices to work smarter across clinical and administrative functions.
Unlike basic automation that follows fixed rules, AI learns from data and adapts its performance over time.
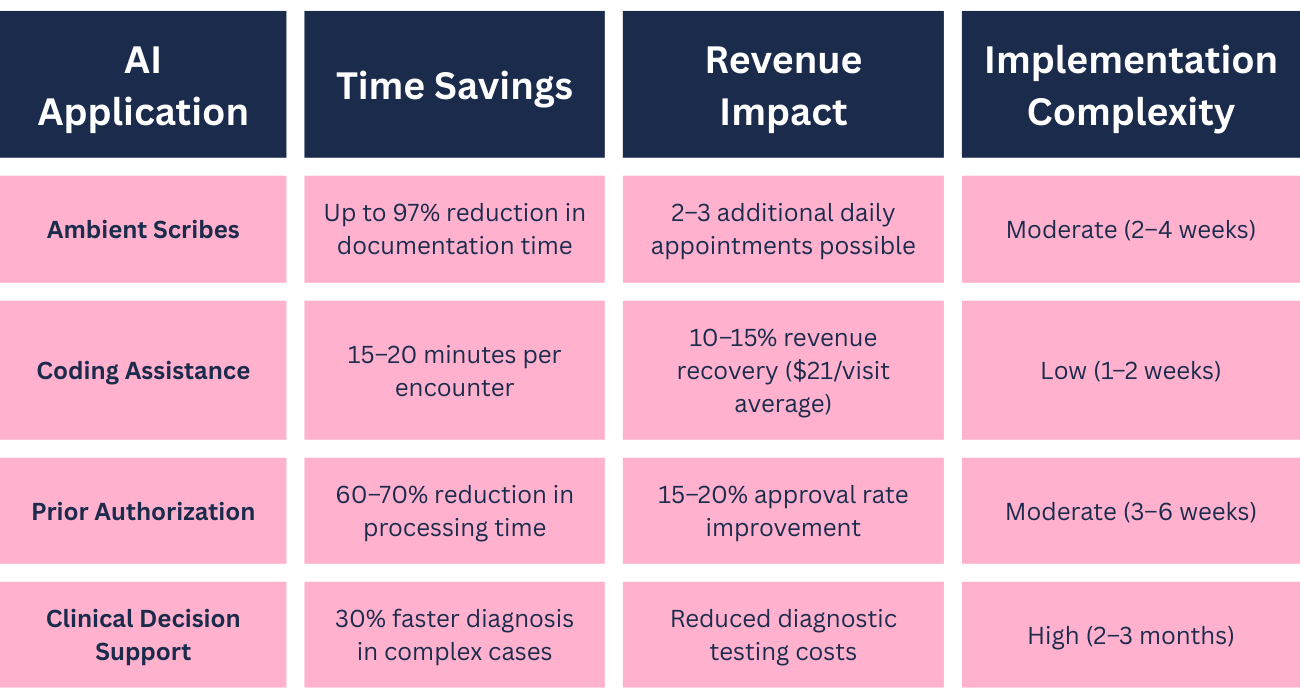
Ambient AI scribes represent one of the most transformative applications for private practices. These systems listen to patient encounters, extract relevant clinical information, and generate documentation in real time. Studies show ambient AI scribes can reduce documentation time drastically, reclaiming hours that clinicians can redirect toward patient care or additional appointments.
For a typical practice, this translates to seeing 2-3 more patients daily without extending work hours. Revenue optimization through AI-powered coding assistance addresses a pervasive problem in healthcare: under-coding. Many providers document care that justifies higher-level billing codes but select lower codes out of conservatism or time pressure. Coding-assist AI recoups 10-15% in lost revenue, adding approximately $21 per therapy visit by ensuring documentation aligns with appropriate billing codes. For a practice conducting 100 visits weekly, this represents over $100,000 in recovered annual revenue.
AI Application Table
Optimizing Patient Engagement for Better Outcomes
Patient engagement encompasses the strategies and tools that foster active participation in care, strengthen patient-provider relationships, and motivate health-promoting behaviors between appointments. Engaged patients demonstrate better adherence to treatment plans, achieve superior health outcomes, and maintain longer relationships with their providers.
Digital tools have revolutionized engagement possibilities. Remote patient monitoring using smart wearables, blood pressure cuffs, or glucose monitors enables continuous data collection between visits. These devices can trigger automated alerts when metrics drift outside target ranges, enabling early intervention before conditions deteriorate. This proactive approach reduces emergency visits and hospital admissions while giving patients tangible feedback on how their behaviors affect their health. Virtual consultations expand access for patients managing chronic conditions, those with mobility limitations, or anyone balancing care with work and family obligations. Computer vision exams, as demonstrated by Allheartz, can reduce unnecessary in-person visits by up to 50% by enabling remote assessment of conditions like skin issues, wound healing, or physical therapy progress.
AI-powered phone agents can answer patient calls 24/7, schedule appointments, collect co-pays securely through integrated payment processing, and route support inquiries directly to your help desk system. This always-available AI receptionist improves access to your practice, streamlines scheduling and payments, and significantly reduces front desk call volume while maintaining a seamless patient experience.
Patient portals serve as engagement hubs where patients can self-schedule appointments, access test results with explanatory notes, review educational materials tailored to their conditions, and communicate securely with care teams. Practices with robust portal adoption report 30-40% reductions in phone calls and higher patient satisfaction scores, as patients appreciate the convenience and transparency. The engagement strategy should match your patient population's preferences and technical comfort. Offer multiple channels-text, email, portal messages, phone-and use analytics to understand which methods drive the best response rates for different patient segments.
Monitoring Key Performance Metrics to Drive Growth

Key Performance Indicators are measurable values that reveal how effectively your practice achieves critical business objectives. Without systematic KPI tracking, scaling decisions rely on intuition rather than evidence, increasing the risk of misallocated resources or missed opportunities.
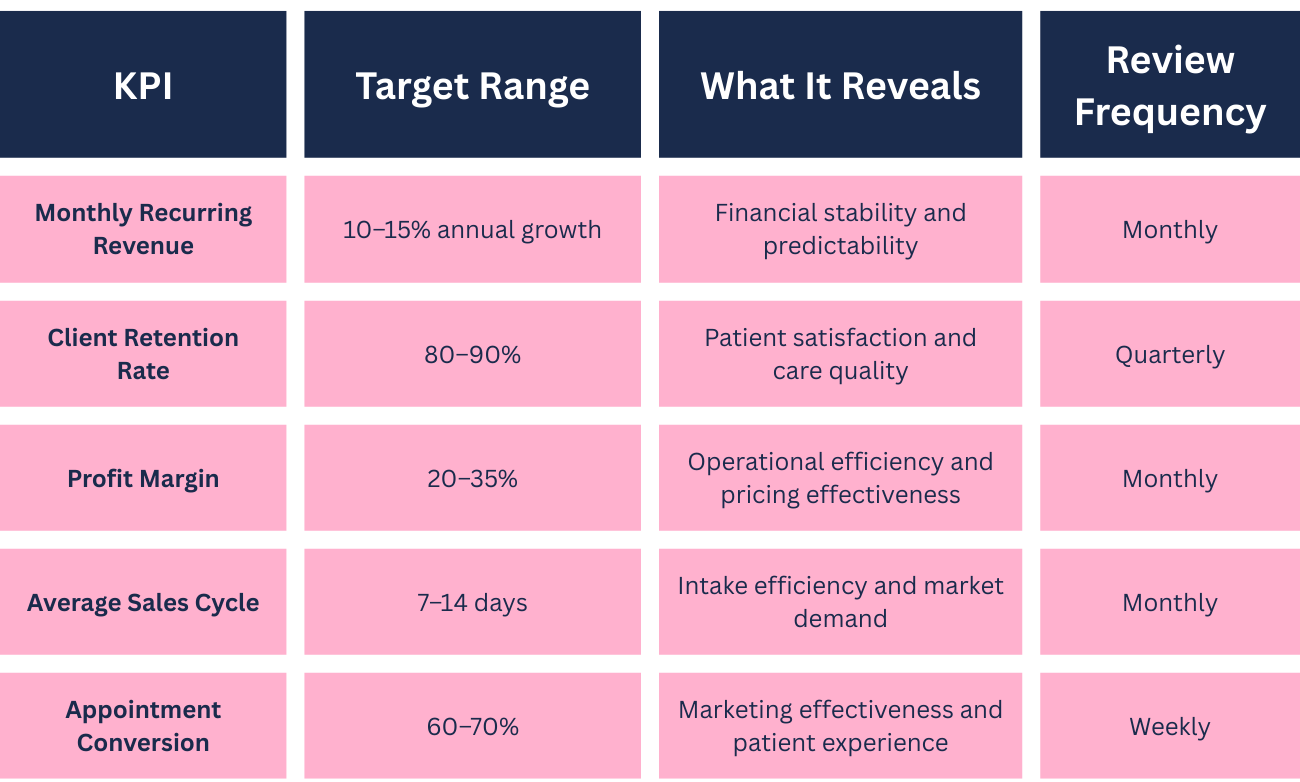
Monthly recurring revenue tracks the predictable income stream from ongoing services, particularly valuable for practices offering membership programs, chronic care management, or subscription-based wellness services. This metric indicates financial stability and helps forecast cash flow during expansion phases.
Client retention rate measures the percentage of patients who return for follow-up care or continue as active patients year-over-year. High retention (above 80%) signals strong patient satisfaction and clinical outcomes, while declining retention warrants immediate investigation into care quality, access issues, or communication gaps. Acquiring new patients costs 5-7 times more than retaining existing ones, making retention a critical scaling metric.
Profit margin, the percentage of revenue remaining after all expenses, determines your capacity to invest in growth initiatives. Healthy private practices maintain margins of 20-35%, with higher margins in specialized or cash-pay services. Track margins by service line to identify which offerings drive profitability and which may need pricing adjustments or operational improvements.
Average sales cycle length measures the time from first contact to completed appointment. Shorter cycles indicate efficient intake processes and strong market demand. If this metric extends beyond industry benchmarks (typically 7-14 days for non-urgent care), examine scheduling availability, insurance verification delays, or communication bottlenecks.
Appointment conversion rate tracks the percentage of inquiries or consultations that result in scheduled appointments. Low conversion suggests issues with pricing transparency, availability, or the initial patient experience. High-performing practices convert 60-70% of qualified inquiries.
KPI Table
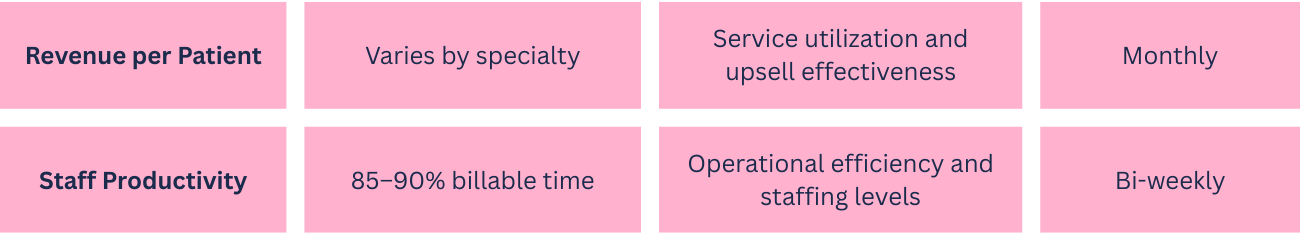
Implement a dashboard that displays these metrics in real-time, enabling quick identification of trends and anomalies. Many practice management platforms, including OptiMantra, offer built-in analytics functions, or you can use business intelligence tools that integrate with your existing systems.
Developing a Strategic Marketing Plan for Client Acquisition
A results-oriented marketing strategy amplifies brand visibility, positions your practice as the preferred choice for your target patients, and creates predictable patient acquisition channels that support scaling goals. Unlike sporadic promotional efforts, strategic marketing operates systematically across multiple channels with clear objectives and measurable outcomes.
Search engine optimization ensures your practice appears prominently when prospective patients search for services you offer. This requires optimizing your website content around the conditions you treat, services you provide, and geographic areas you serve. Local SEO, including Google Business Profile optimization, local directory listings, and location-based content, proves especially valuable for practices drawing from specific communities.
Content marketing establishes your expertise while addressing patient questions and concerns. Blog posts, videos, and downloadable guides that explain conditions, treatment options, and wellness strategies attract prospective patients in research mode. This content also supports SEO efforts and provides material for social media and email campaigns. Focus on topics that align with your highest-value services or areas where you want to grow.
Email campaigns nurture relationships with both prospective and existing patients. Segment your lists to deliver relevant content: educational series for new subscribers, appointment reminders and health tips for active patients, and re-engagement campaigns for those who haven't visited recently. Automated email sequences can onboard new patients, follow up after appointments, and promote seasonal services or new offerings.
Social media engagement builds community and keeps your practice top-of-mind. Rather than broadcasting promotional messages, share valuable health information, behind-the-scenes glimpses of your practice culture, and patient success stories (with permission). Platforms like Instagram and Facebook work well for visual health content, while LinkedIn suits practices targeting professional networks or B2B referral sources.
Define ideal patient personas before launching campaigns. Detail their demographics, health concerns, decision-making factors, and information sources. This clarity ensures your messaging resonates and your marketing budget targets the highest-probability prospects. A weight management practice might target health-conscious professionals aged 35-55 who value convenience and evidence-based approaches, while a pediatric practice focuses on new parents seeking developmental support and preventive care.
Marketing automation platforms orchestrate these efforts, tracking which campaigns generate appointments, calculating cost-per-acquisition by channel, and automatically nurturing leads through multi-touch sequences. This data-driven approach allows continuous optimization, shifting resources toward the highest-performing channels.
Building and Managing a Team That Supports Expansion

Your team represents the most critical scaling resource. While technology and systems enable efficiency, people deliver the personalized care and judgment that define exceptional practices. Strategic team building ensures you have the right capabilities, clear accountability, and a culture that sustains growth.
Start by documenting clear roles and responsibilities for each position. Ambiguity around who handles specific tasks creates inefficiency, duplication, and gaps where critical work falls through cracks. As you scale, specialization becomes increasingly valuable - front desk staff focused on patient experience, dedicated billing specialists, clinical support staff handling routine protocols, and providers concentrating on diagnosis and treatment planning.
Recruitment should prioritize cultural fit alongside technical skills. Candidates who align with your practice values, communication style, and patient care philosophy integrate more smoothly and stay longer. Develop a structured interview process that assesses both competencies and cultural alignment, including scenarios that reveal how candidates handle common challenges in your environment.
Onboarding sets the foundation for new team member success. Comprehensive orientation covering clinical protocols, technology systems, communication standards, and practice culture accelerates productivity and reduces early turnover. Assign mentors or buddies who can answer questions and provide informal guidance during the first 90 days.
Leadership development ensures you're not the bottleneck as the practice grows. Identify high-potential team members and invest in their management capabilities through training, increasing responsibilities, and regular coaching. Building a leadership layer between you and frontline staff enables you to focus on strategy rather than daily operations.
Regular check-ins maintain alignment and surface issues before they escalate. Weekly team huddles review upcoming schedules and priorities, monthly one-on-ones provide individual feedback and development discussions, and quarterly all-staff meetings communicate practice performance and strategic direction. These touchpoints reinforce accountability while demonstrating your investment in team member growth.
Professional development opportunities - whether continuing education, conference attendance, or cross-training in new skills - improve capabilities while signaling that you value team members' career progression. This investment pays dividends in retention, as talented staff are more likely to stay when they see pathways for growth within your practice.
Establishing Effective Referral Programs to Increase Patient Volume
Referral programs create structured systems that reward existing patients or professional partners who introduce new patients to your practice. Unlike passive word-of-mouth, active referral programs systematically generate patient flow without the high cost of traditional advertising.
Patient referral programs incentivize your satisfied patients to recommend your services to friends and family. Incentives might include service discounts, complimentary add-on treatments, or charitable donations made in the referring patient's name. The key is making the process simple - provide referral cards, create a dedicated landing page for referred patients, and automate tracking so you can thank referrers promptly.
Professional referral networks with other healthcare providers generate high-quality patient flow. Primary care physicians, specialists in complementary fields, physical therapists, nutritionists, and mental health providers all serve patients who may benefit from your services. Building these relationships requires identifying natural referral partners, educating them about your services and ideal patient profiles, and creating easy referral pathways - whether electronic referral systems, dedicated phone lines, or liaison staff who facilitate handoffs.
The most successful professional referral programs operate reciprocally. When you refer appropriate patients to partners, they're more likely to reciprocate. Track referral patterns to ensure balanced relationships and identify partners who consistently send appropriate patients.
Communication templates streamline referral program execution. Develop email or letter templates that introduce your practice to potential professional partners, thank patients for referrals, update referring providers on patient progress (with appropriate consent), and periodically remind your network about your services. Automation tools can trigger these communications at appropriate intervals without requiring manual effort.
Measure referral program performance by tracking referral sources, conversion rates from referral to appointment, and lifetime value of referred patients. This data reveals which referral channels deliver the highest return and deserve increased investment.
Implementing Scalable Technology and Practice Management Tools
Scalable technology refers to software and platforms that accommodate increasing workload, users, and data volume without performance degradation or requiring complete system replacement. As your practice grows from 10 to 50 to 200 daily appointments, scalable systems maintain speed, reliability, and functionality.
Robust practice management and EHR/EMR platforms serve as the operational backbone for scaled practices. These integrated systems should handle automated scheduling with online booking, patient reminders, and waitlist management; comprehensive electronic health records with customizable templates and clinical decision support; billing and revenue cycle management with automated claim submission and denial tracking; and analytics dashboards that surface key performance metrics in real-time.
Performance analysis tools like Apache JMeter test software scalability by simulating high user loads and identifying bottlenecks before they affect patient care. When evaluating practice management platforms, ask vendors about their scalability testing, maximum concurrent users, and performance guarantees as your practice grows.
Look for platforms with robust API capabilities that enable integration with specialized tools such as lab systems, imaging centers, patient engagement apps, or financial software. These integrations eliminate duplicate data entry, reduce errors, and create seamless workflows across your technology ecosystem. OptiMantra's direct lab integrations exemplify this approach, enabling providers to order tests, receive results, and review trends without leaving the primary platform.
Core Feature Comparison Table
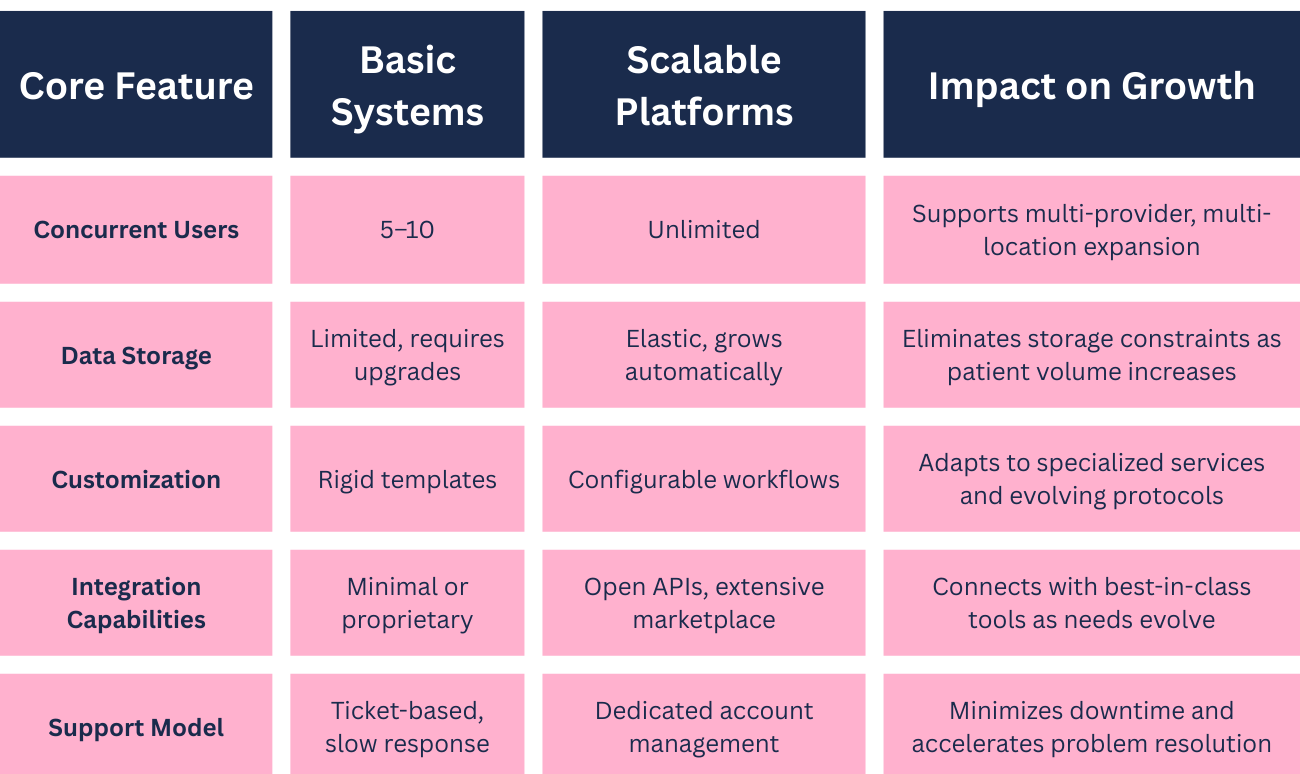

Cloud-based systems offer inherent scalability advantages over on-premise software. They eliminate hardware maintenance, provide automatic updates, enable remote access for telemedicine or multi-location practices, and typically offer better disaster recovery and security than most practices can implement independently.
When selecting technology partners, prioritize vendors with proven track records supporting practices at your target size. Ask for references from practices that have scaled successfully using their platform, and understand their product roadmap to ensure continued innovation aligns with your growth trajectory.
Applying Frameworks and Methodologies for Sustainable Growth
Scalability frameworks provide structured methodologies for designing operations and processes that expand smoothly with increasing demand. Rather than ad hoc growth that strains systems and people, frameworks ensure expansion follows proven patterns that maintain quality and efficiency.
The Scaled Agile Framework (SAFe) represents the most widely adopted agile scaling methodology, originally developed for software development but increasingly applied to healthcare operations. SAFe emphasizes team coordination across multiple groups working toward common objectives, strategic alignment ensuring all efforts support overarching practice goals, and continuous improvement through regular retrospectives and process refinement.
For private practices, SAFe principles translate to coordinating clinical, administrative, and business development teams around patient experience and practice growth objectives. Regular planning sessions align these groups, while daily standups and sprint reviews maintain momentum and surface obstacles quickly. This structured approach prevents the chaos that often accompanies rapid growth.
Implementing these frameworks begins with leadership commitment and training. Bring in experienced coaches who can tailor the methodology to healthcare contexts, train your team in the relevant practices, and guide initial implementation. Start with one service line or location as a pilot, refine the approach based on lessons learned, and then scale the framework across the broader practice.
The discipline these frameworks impose - regular planning, clear accountability, systematic problem-solving - prevents the reactive firefighting that undermines many scaling efforts. Teams know what success looks like, understand their role in achieving it, and have forums to address obstacles before they derail progress.
Ensuring Legal Compliance and Risk Management During Scaling
Risk management involves systematically identifying, assessing, and mitigating potential legal, financial, and operational hazards that could harm your practice. As you scale, risk exposure increases - more patients, more staff, more locations, and more complex operations all create additional vulnerability.
Healthcare regulatory compliance tops the risk list. HIPAA privacy and security rules apply regardless of practice size, but enforcement scrutiny and potential penalties scale with patient volume and data breaches. As you grow, implement comprehensive HIPAA compliance programs including regular staff training, technical safeguards like encryption and access controls, business associate agreements with all vendors handling protected health information, and incident response plans for potential breaches.
State and federal healthcare laws govern everything from scope of practice and supervision requirements to fraud and abuse prohibitions. Multi-state practices face additional complexity navigating varying state regulations. Engage healthcare attorneys to review your compliance posture as you expand, particularly when adding new services, crossing state lines, or changing business structures.
Staff credentialing and privileging processes must scale with your team. Verify licenses, certifications, and malpractice coverage for all clinical staff, and implement systems that track renewal dates and continuing education requirements. Automated credentialing platforms reduce administrative burden while ensuring no gaps in coverage.
Professional and general liability insurance needs increase with practice size and service diversity. Review coverage annually with an insurance broker specializing in healthcare practices, ensuring policy limits match your risk profile and that all locations, providers, and services are appropriately covered. Consider umbrella policies that provide additional protection beyond primary coverage limits.
Regular compliance audits identify vulnerabilities before the





